For the first time in years, fewer people are signing up for health insurance through the Affordable Care Act (ACA) Marketplace known in Kentucky as kynect. Early data from the 2026 open enrollment period show that Marketplace plan selections are down compared with the same point last year. According to KFF, Marketplace enrollment is falling for the first time after several years of steady growth and record participation, and it comes as the cost of Marketplace coverage has risen sharply.
The Marketplace is how millions of people across the U.S., and nearly 100,000 Kentuckians, get health insurance when they do not have access to coverage through a job, Medicare, Medicaid, or military benefits.
Marketplace Enrollment Is Falling as Monthly Costs Rise
According to the Centers for Medicare and Medicaid Services (CMS), 23 million people nationwide signed up for Marketplace coverage during the 2026 open enrollment period, which ended January 15th, including more than 86,000 in Kentucky. This is in comparison to 24 million Americans and 97,000 Kentuckians in 2025.
This drop in enrollment follows rising base premium rates compounded by the expiration of enhanced premium tax credits at the end of 2025. These subsidies lowered monthly premiums for Marketplace enrollees in 2025.
What the Premium Data Show
To understand why enrollment is falling, it helps to look at actual plan prices. One of the easiest measures to understand is the average benchmark premium, which is the price of the second-lowest-cost Silver tier plan in each state before any financial help is applied. These benchmark premiums set the starting price of Marketplace coverage and are used to calculate premium tax credits.
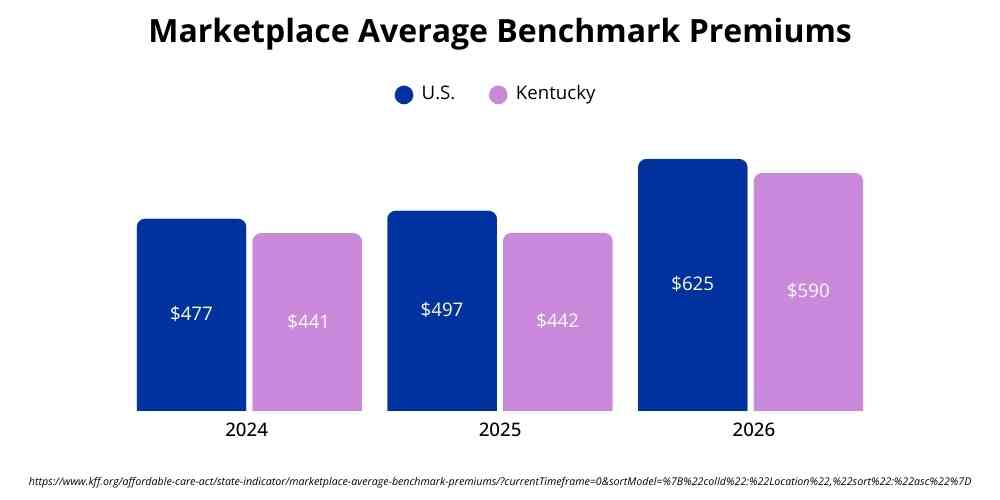
According to KFF’s state-by-state Marketplace pricing data, benchmark premiums for 2026 are higher than in recent years across most of the country. Nationally, the average benchmark premium is now $625 per month for a typical adult before subsidies are applied. In Kentucky, the benchmark premium increased by one-third, from $442 in 2025 to $590 per month in 2026.
This means that Marketplace plans now begin at prices many households simply cannot afford. Families who once qualified for premium help no longer qualify. Because of that change, some families are seeing their yearly costs more than double, with increases reaching as high as 114%.
Higher Prices, Fewer Enrollees
For some, these higher costs mean delaying enrollment. For others, it means not enrolling at all. The early 2026 enrollment data reflect these decisions. It’s not that people don’t need the coverage; they just can’t afford it.
TAI’s 2024 survey of 1,001 adult Kentuckians found that due to medical costs, 57% avoided, skipped, or stopped medical care or medications, and 40% were unable to buy food or clothing. When health needs arise, people need to be able to obtain care without risking other essential needs.
Why This Is a System Problem, Not an Enrollment Problem
The KFF Marketplace data points to a bigger problem. In the U.S., health insurance is something people have to qualify for, sign up for, and pay for every year. Even after they enroll, they still face extra costs each time they see a doctor or get medical care.
This problem would not exist under a universal health care system. Coverage, and the cost of coverage, would not depend on age, employment, income thresholds, annual enrollment periods, arbitrary measures of “deservedness,” political whims, or by companies whose goal is to make a profit rather than to provide care. Families in Kentucky and across the country would have stable access to care without having to make yearly decisions about whether they can afford to stay insured or use the coverage they have.
The Bottom Line
The early 2026 data are worrisome for the health and well-being of our country. As Marketplace premiums have risen and Congress has failed to renew the enhanced premium tax credits, fewer people are enrolling in coverage. National average benchmark premiums now exceed $600 per month, and Kentucky’s are close behind, pricing people out of the system. When cost is a barrier, care is lost, and physical, emotional, and financial suffering increase.

